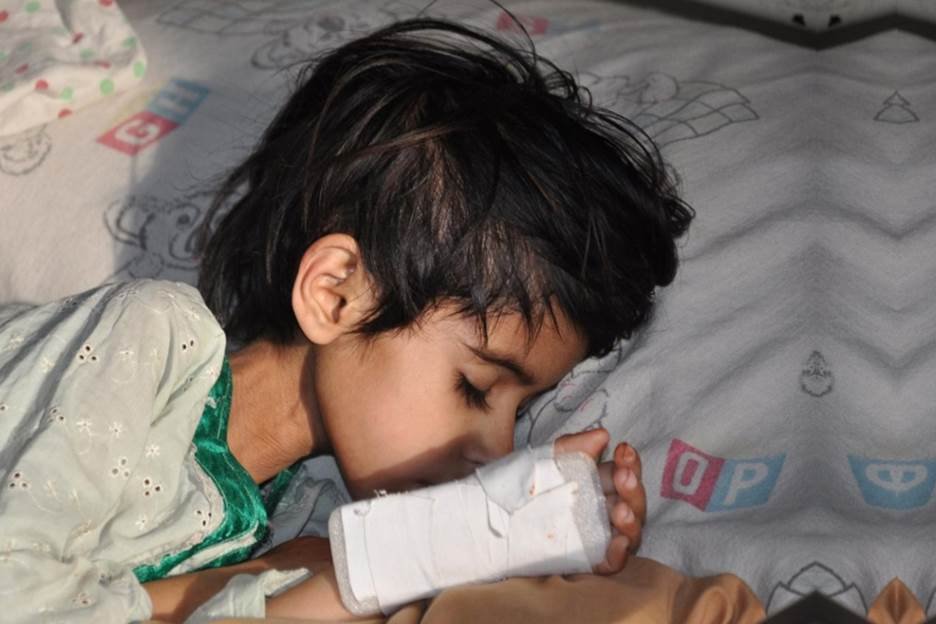
In a lot of villages across sub-Saharan Africa, South Asia, and parts of Latin America, women give birth at home because there is no real alternative. The clinic is hours away. The road washes out. The money is already gone. Someone nearby steps in and helps. Usually it goes fine. Sometimes it doesn’t.
This is not unusual. This is just how it is in places where healthcare is more of a promise than a reality. Most of these births go unrecorded. Most of these close calls go uncounted.
One international nonprofit has been working in exactly these places for more than ten years. They just announced they’re moving into more regions.
What “Expansion” Actually Means Here
Nobody’s cutting a ribbon here. No press release, no new office, no big moment. When this organization says it’s expanding, what that actually means is more dirt roads, more waiting, more knocking on doors that don’t open right away.
A coordinator drives four hours to talk to a village council. That might lead somewhere, or it might take three more visits. A training that should take a week stretches into three because that’s how it goes. A batch of malaria tests sits in a storage room while everyone waits on one signature from a district office that’s been quiet for a month and a half.
This is what the work looks like up close.
The people carrying most of it are community health workers. Locals. People who already live in these communities and got trained to handle basic care at home. There are no doctors in most of these places, so the question was never about replacing anyone. It was just about whether there would be something, or nothing at all.
The People Doing the Actual Work
Nobody recruited heroes for this. They recruited neighbors. That’s the whole idea. They come from the communities they serve. They know the roads, the families, the local politics of who talks to whom. The organization trains them, hands them supplies, and pays a small monthly stipend. Then they go to work. What that looks like day to day is walking. A knock on a door. A pregnant woman at seven months who needs someone to show up. A child who had malaria two weeks ago and still isn’t quite right. Reminding a household that vaccine day is coming. Writing it all down and handing the notebook to a supervisor every couple of weeks. That’s it. No clinic. No doctor. Just someone who lives nearby and knows what to look for. Organizations doing this kind of work at scale, like those running community health workers in underserved regions and they aren’t building hospitals. They’re making sure someone shows up.
Where the Work Is Expanding and Why Those Places
The new regions being brought into the program share a few things in common. High rates of child death. High rates of mothers dying during or after childbirth. Low rates of people actually getting any care at all, even basic care.
A district in northern Nigeria was recently added to the program. Surveys done there found that under 30 percent of women had seen anyone with formal health training during their last pregnancy. Not a doctor. Not a nurse. Not a midwife. Just whoever happened to be there, a relative, someone from the village, or a traditional birth attendant with no formal background. That was it.
That number tells you everything about the kind of gap being addressed.
The organization does not pick regions based on ease of access or political convenience. It picks them based on need. Which also means it picks some of the hardest places to work in.
Pregnancy and Early Childhood Are the Core Focus
It doesn’t matter who you ask in global health. The answer comes back the same. Most of the deaths that didn’t have to happen, happen during pregnancy, during childbirth, or somewhere in a child’s first five years.
So that’s where the program focuses.
Health workers stay close to pregnant women through the whole stretch. Showing up, checking in, making sure warning signs don’t get ignored, making sure someone is around when labor starts. And after the baby arrives they keep coming, because the danger doesn’t stop at delivery.
With young children the approach is basic and practical on purpose. Nutrition. Vaccines. Getting ahead of pneumonia and diarrhea before they turn serious. Both of those infections are still killing huge numbers of children every year in poorer regions, which is genuinely hard to sit with when you know that both are treatable. The medicines are cheap. They’ve existed for decades.
The issue was never finding a cure. It’s that the cure isn’t in the room when the child needs it.
What Happens When the Supply Chain Breaks
Here is something that does not make it into most nonprofit annual reports. Programs fail quietly, sometimes, because of logistics.
A health worker is trained, motivated, ready to work. But the malaria test kits have not arrived. Or they arrived but expired during the delay. Or the clinic that was supposed to receive referrals is closed three days a week because it only has one nurse and she is the one who also runs the immunization outreach.
The organization has run into all of these. Supply chain management, which sounds dry, is actually one of the most critical parts of making community health work function. Getting basic medicines and diagnostic tools into remote areas reliably is harder and more expensive than it looks from the outside.
The expansion includes investment in this area specifically. Stronger local procurement where possible, better tracking systems, and relationships with district health offices that help move things through bureaucratic delays a little faster.
Working With Government, Not Around It
One of the reasons many health programs in low-income regions do not last is that they operate in a parallel universe next to the government system, rather than inside it. When funding ends, everything they built vanishes.
This organization tries to avoid that pattern. It works alongside national health systems, not instead of them. Health workers are trained within the framework of national standards. Data goes into government health records. Referral pathways connect to government clinics.
This approach is slower. Government systems have their own pace. And then there’s everything else. The paperwork. The meetings. The people who have the authority to say yes and keep saying not yet. None of that is fast.
But it is the difference between a program that lasts and one that does not.
In several countries where the organization has been working for five or more years, it is now advocating for community health workers to be formally employed and paid by the government. When it gets to that point, nobody needs to hold it up anymore. It just stands.
Clean Hands, Clean Water, and Sick Children
Diarrhea in a child is not complicated to treat. Oral rehydration salts, monitoring, rest. What is not straightforward is treating the same child for diarrhea again three weeks later, because the water source they drink from is shared with livestock and sits ten meters from where the family uses as a toilet.
This is the reality in a number of the communities the program serves. And it is why the expansion in some areas includes basic hygiene and sanitation work alongside health care.
The organization is not building water systems. That is a different kind of program with different expertise. What it does is train health workers to talk about handwashing, to help communities identify and protect cleaner water sources, and to connect hygiene behavior to the health outcomes families actually care about, like keeping children from getting sick repeatedly.
Small changes at this level, practiced consistently, reduce the return rate of illness significantly. The data on this is not new or controversial. It just takes effort to make it happen in practice.
When Communities Do Not Trust You Yet
In a village in eastern Uganda, the program spent four months before a single household agreed to regular health worker visits.
The reason was not hostility. It was an experience. An NGO had come through years before, taken surveys, made promises about a new health post, and never returned. People remembered. They were not going to open up to strangers again without some evidence that this time was different.
So the team showed up. Every week. Sometimes just to talk, not to deliver any health services at all. They helped with a community event. They fixed a small problem with a water point that the previous NGO had surveyed but done nothing about. They did not announce anything.
By month five, a grandmother asked if a health worker could check on her daughter who was eight months pregnant.
That was the beginning. Today, that village has one of the higher antenatal care rates in the district. Trust, once built, tends to hold. Getting there is just not fast and not guaranteed.
Data Collection and What It Actually Reveals
Every visit gets recorded. Not in a database, not always. In many areas, it is still a paper form in a notebook. But those forms get collected, entered, and reviewed.
The numbers that come back from established areas are encouraging. Where the program has had time to settle in, three years or more, the number of children dying from preventable causes has gone down. The share of pregnant women getting care has gone up. More children are seeing their vaccinations through to the end..
But the organization is careful about how it presents these results. Health outcomes are shaped by many things at once, not just a single program. Economic changes, rainfall, road improvements, a new government initiative, all of these affect health. Claiming full credit for improvements would be misleading.
What the data does show, clearly, is uptake. People are using the service. That alone is significant in places where health care was previously not available at all.
Mobile Phones Are Helping, Carefully
In some regions, health workers now use basic mobile phones to log visits and flag urgent cases. The system is simple on purpose. It works on cheap handsets with weak signal. It does not require the internet.
Supervisors can see at a glance which areas have not had a logged visit recently, or which health workers might need support. Supply shortages get flagged earlier. Some referrals get confirmed by phone before a patient makes the trip to a distant clinic, which saves time and money for families operating on tight margins.
The organization is thoughtful about what it introduces and when. A digital tool that workers do not understand or trust just creates extra work. Rollout is slow, with training, with feedback, with adjustments.
What This Kind of Work Costs and Who Pays For It
Community health programs are not expensive relative to other health interventions. Training a health worker, supplying them, and supervising them for a year costs a fraction of what a single hospital bed costs in a high-income country.
None of this is free to run. The money comes from private donors, foundations, and government grants, usually some mix of all three. That’s by design. An organization that leans too hard on one big donor is always one decision away from having the whole thing fall apart.
The longer-term goal is government co-financing. Getting health ministries to contribute to the cost of CHW programs is part of every country-level conversation the organization has. It is not always successful. Budgets are tight and priorities compete. But each year more governments are moving in this direction.
The Honest Assessment
This is useful, real work. It is also incomplete, underfunded, and operating in conditions that make every step harder than it should be. The nonprofit knows this. The people who work in it know it better than anyone. They go back anyway, because the communities they serve have no other option if they don’t. That is the thing about programs that actually last. They are not the ones with the cleanest reports or the most impressive launch days. They are the ones that tell you what went wrong and come back the next week. That is the standard any humanitarian charity supporting vulnerable communities should be held to.